Recurrent patellar dislocation is a condition characterised by the repeated slipping of the patella, or kneecap, out of its groove on the front of the lower end of the femur (thigh bone). When the patella dislocates on more than one occasion the term ‘recurrent patellar dislocation’ is used.
Unlike a subluxation, where the patella partially dislocates but immediately returns to its place, a true patellar dislocation involves a distinct movement, typically occurring when the knee is straightened.
The chance of another dislocation after the first occurrence is immediately heightened, ranging from 15% to 45%. This risk escalates further after subsequent dislocations, reaching approximately 60% to 80% after two occurrences. Various predisposing factors, including leg alignment, patellar positioning, and foot and ankle alignment, contribute to this condition.
It’s crucial to differentiate between a patella dislocation and a knee dislocation. A patella dislocation specifically involves the displacement of the kneecap itself. On the other hand, a knee dislocation extends beyond the patella to include misalignment between the thighbone (femur) and the shinbone (tibia). Unlike patella dislocations, knee dislocations are relatively uncommon and more severe due to the significant force required to disrupt the alignment of the leg bones, often resulting in damage to the surrounding ligaments.
Recurrent patella dislocation can stem from a variety of factors, including certain inherited traits such as a kneecap positioned too high within its groove or a shallow trochlear groove.
Additionally, tight ligaments surrounding the knee and a valgus leg alignment (knock-kneed legs) can contribute to this condition. Trauma, whether from twisting or bending motions, also poses a risk factor, particularly in children and teenagers as their bones are still developing.
Each instance of dislocation exacerbates the issue by stretching soft tissues, further heightening the likelihood of recurrence.
Other factors that may contribute to recurrent patellar dislocation are:
The common symptoms of recurrent patella dislocation include:
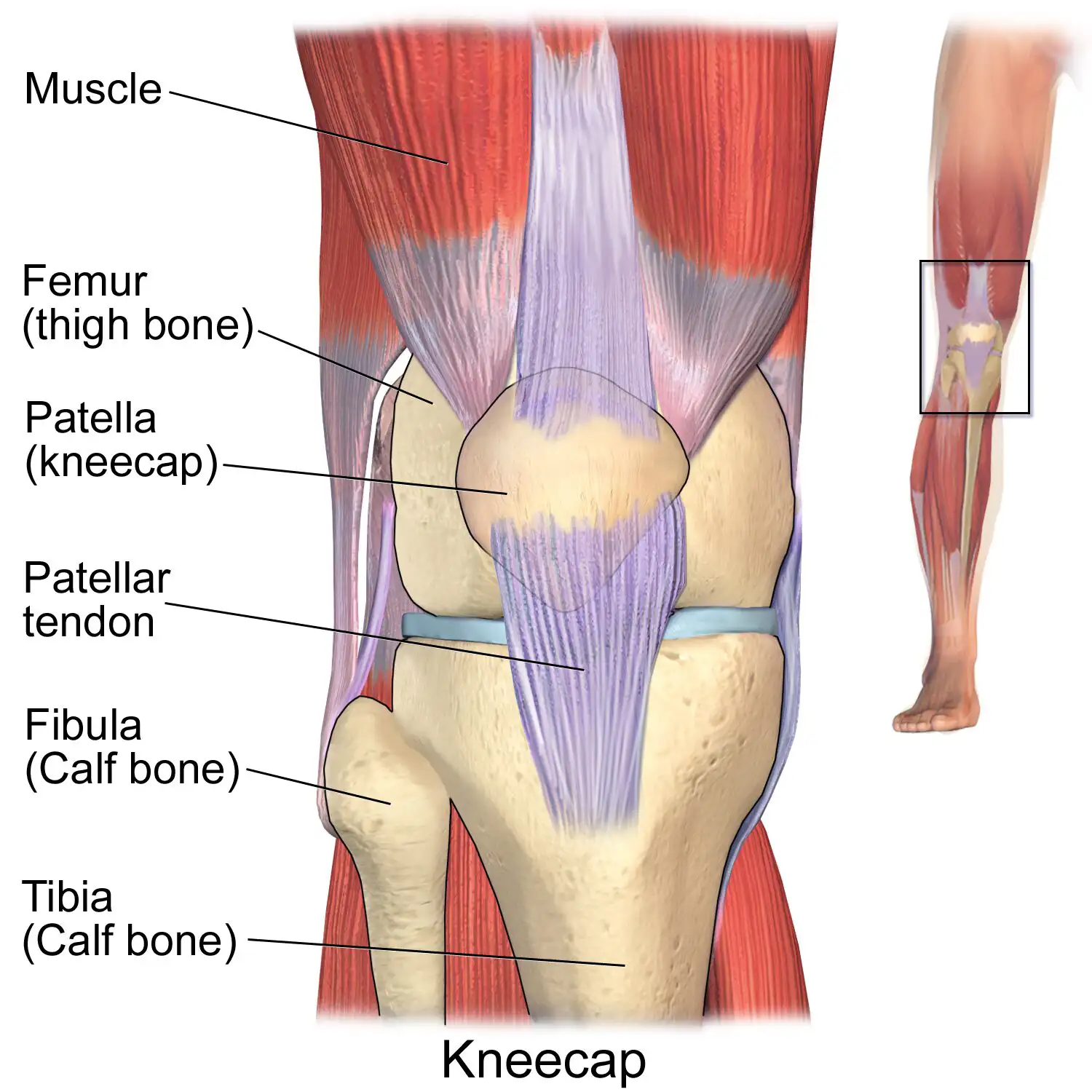
The knee joint is a complex structure comprising several major components. The patella, or kneecap, is a triangular bone located in front of the knee joint that protects the joint and aid in movement. It interacts with the femur (thigh bone) and the tibia (calf/shin bone) to form the knee joint.
Surrounding the knee are the quadriceps muscles, including the rectus femoris, vastus lateralis, vastus medialis, and vastus intermedius, which play a crucial role in straightening the knee and stabilising the patella during movement.
The patellar tendon connects the bottom of the patella to the tibia. Ligaments such as the medial patellofemoral ligament (MPFL) and the lateral patellofemoral ligament (LPFL) contribute to patellar stability, with the MPFL located on the inner side and the LPFL on the outer side of the knee.
Within the knee joint, articular cartilage covers the ends of the femur, tibia, and patella, providing a smooth surface for movement and cushioning the bones during weight-bearing activities. The meniscus, a C-shaped cartilage structure between the femur and tibia, acts as a shock absorber and helps distribute load within the knee joint.
For people experiencing a patella dislocation once or twice, and with minimal predisposing factors, non-surgical treatment may be the recommended course of action.
Non-surgical treatments for patella dislocation typically focus on strengthening the muscles around the knee joint and improving flexibility to stabilise the patella. This often involves targeted exercises to strengthen the quadriceps, with particular emphasis on the vastus medialis obliquus (VMO) muscle, which plays a crucial role in patellar stability.
Additionally, stretching exercises may be prescribed to improve the flexibility of structures around the knee, such as the iliotibial band (ITB/IT Band) and the lateral retinaculum. Orthotic interventions, such as braces or shoe inserts, may also be recommended to optimise foot and ankle alignment and reduce stress on the knee joint.
Overall, non-surgical approaches aim to address underlying muscular imbalances and biomechanical issues to prevent recurrent patella dislocations and promote long-term joint health and stability.
When surgery becomes necessary, a range of options tailored to each patient’s unique anatomy and age are considered. Surgical options for recurrent patella dislocation encompass various procedures aimed at realigning and stabilising the patella within the knee joint.
Advanced imaging techniques such as X-rays, CT scans, or MRIs guide surgical decisions by providing detailed insights into knee and patella alignment. Typically, surgical interventions involve arthroscopic procedures to address bone surface irregularities and remove any intra-articular debris.
During surgery, meticulous attention is given to reconstructing the MPFL (Medial Patellofemoral Ligament), a ligament often compromised during initial dislocation events. Reconstruction techniques may involve utilising hamstring tendon grafts secured with screws or anchors, strategically placed through drill holes in both the patella and femur.
In cases where patellar height poses an issue, adjustments to the tibial tuberosity (bony prominence on the upper shin where the patellar tendon attaches) may be made to reposition the patella downwards. It is fixated using screws that may require removal in future. Medial or distal shifts of the tibial tuberosity can also be made if necessary.
Although less common, trochleoplasty procedures aimed at augmenting the patellar groove on the femur are also an option. This involves removing bone and reshaping the groove to better accommodate the patella.
Overall, the choice of surgical option depends on factors such as the patient’s age, knee and patella alignment, and the severity of the condition, with the goal of restoring patellar stability and function while reducing the risk of future dislocations.
Whatever surgery has been performed, there is always a risk of further episodes of patellar dislocation. The risk of a further dislocation is usually less than 10% but the nature of the condition means that we cannot reduce it to 0%.